What is a kegel?
Simply put, a kegel is an engagement of the pelvic floor muscles. It has been found through substantial research to be effective at curing or improving urinary incontinence. There is also ongoing research into kegeling as a treatment for pelvic organ prolapse.
Kegel 2.0 vs. “Kegeling”
Before we go further, I want to distinguish between engaging the pelvic floor muscles and “squeezing like you’re trying not to pee.” The pelvic health community has started to steer away from prescribing “kegels,” as they’ve largely been over-simplified and too broadly recommended. If all you ever did for your pelvic health was squeeze the urethral sphincter, that could easily do more harm than good.
Instead, I teach what I call the Kegel 2.0, which differs from a “kegel” in that it focuses on using the entire pelvic floor, and prioritizes releasing pelvic floor engagement as highly as creating it. In order for that distinction to make sense, we’ll need to jump into some more detail:
Kegels: A brief history
Kegels are named for the gynecologist, Dr. Arnold Kegel, who did not actually invent the idea of engaging your pelvic floor (but gets all the credit for it). In fact, the idea has been around for thousands of years in traditional cultures. In modern times, Kegel was actually preceded by over a decade by another researcher. However, Kegel’s research was instrumental in bringing awareness to the idea of using pelvic floor engagement as a non-surgical alternative for treating incontinence, so we’ll still give him a little credit. You can learn more about the fascinating history of the kegel here.
Anatomy of a kegel
My husband likes to joke that “the pelvic floor has something to do with linoleum vs. tile, right?” In fact, your pelvic floor is the hammock or bowl of muscles inside your pelvis that basically keeps your insides inside. There are 3 layers of pelvic floor muscles, some of which we can consciously control (the outermost layer) and some of which we can’t (the inner layers). Fortunately, when we practice engaging the superficial or outermost pelvic floor muscles (and deep, transverse abs), the deeper layers tend to come along for the ride.
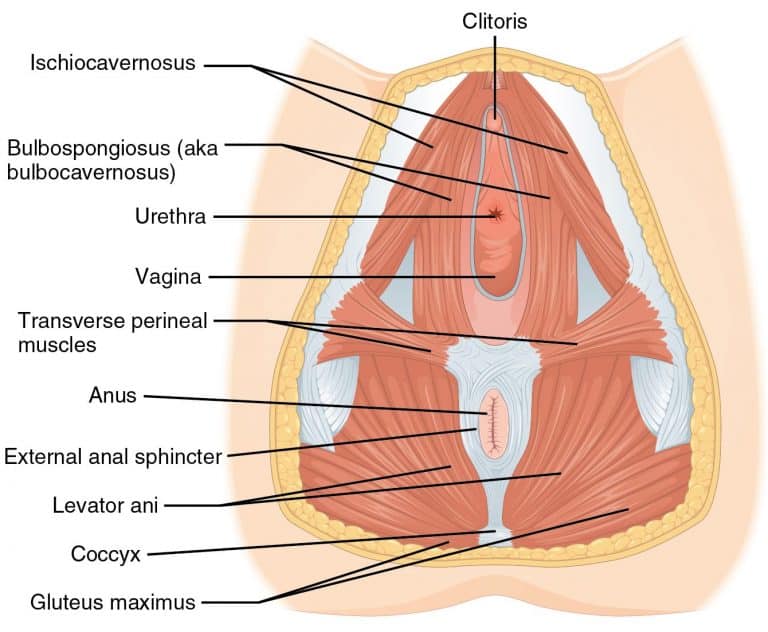
The superficial pelvic floor muscles connect between the pubic bone at the front of the pelvis, the tailbone at the back, and the sit bones on the right and left. One set of muscles makes a diamond between these points, while another set makes a figure-8 around the vaginal opening and urethra at the front and the anus in the back. To engage these muscles, you can think about drawing the sit bones, pubic bone, and tailbone toward each other.
Why should you kegel?
The most important thing to understand about kegeling is that not everyone should. While most women (especially postpartum) are concerned their vagina and pelvic floor will be too loose, as much as 40% are actually too tight. Learn whether your pelvic floor is too loose or too tight right here.
If you’re too tight, you actually do not want to practice kegels, but rather focus on releasing the pelvic floor, stretching the muscles of the pelvic floor, and neurologically repatterning the way you hold tension in your abs and pelvic floor. If you’re too loose in the pelvic floor, then kegels are a great idea in combination with other pelvic floor and full-body exercises. Check back here in a few weeks for a full list of exercises for hypotonic pelvic floors.
Does kegeling help with…
Kegeling can be a component in a recovery program for many different pelvic issues. Below are just a few examples where they may or may not help. Of course, you should always consult a physician or pelvic floor PT before attempting to heal any of the below with an at-home program.
- Diastasis recti (DR): A DR is a separation of the connective tissue of the 6-pack or rectus ab muscles. Effectively engaging the pelvic floor when doing corrective ab exercises is essential in order to prevent prolapse or other symptoms when recovering a DR.
- Pelvic organ prolapse (POP): Kegels are being researched as one potential treatment for prolapse. While they may not work alone, they are one helpful component in a prolapse recovery program.
- Pelvic floor hypertonicity: As described above, kegels are not appropriate when you have a hypertonic pelvic floor. Some of these exercises may be a good idea.
- Vulvodinia: Vulvodinia is often caused by an overtight pelvic floor. As such, kegeling would not be recommended to help resolve this issue.
- Ischial bursitis or weaver’s bottom: As above, ischial bursitis may be caused by hypertonicity, so kegeling would not be recommended without the guidance of a pelvic floor PT.
- Symphysis pubis dysfunction (SPD): SPD is caused by a laxity in the bones and joints of the pelvis. While pelvic floor hypotonicity alone is probably not to blame, kegeling may be one component in a SPD treatment plan.
- Tailbone pain: Depending on the cause of tailbone pain, kegeling might not be a great idea. If you were to kegel, you would want to be sure you aren’t over-tightening the tissue immediately around the tailbone.
- Urinary leaking: Depending on whether your pelvic floor is too loose or too tight, kegeling might not help. You should first figure out whether your pelvic floor is loose or tight.
As you can see, pelvic floor engagement may or may not be recommended dependent on a wide array of factors. If your head is spinning with the potential courses of action, I encourage you to shoot me a message or book a free wellness consult. Let’s get to the root of your root issues!